Surgical Gown vs Isolation Gown? What are the differences?
To help you choose the right gown, we take you through all the fundamentals and the key things in selecting the best one.
As the COVID-19 outbreak continues, the use of isolation gowns is now becoming popular among the public. They are part of personal protective equipment (PPE). In this time of the pandemic, the demand for gowns from the public is also increasing. Because the rise of the virus spread is becoming more threatening. It gives us more reasons to find simple alternatives to fight the virus. Isolation gowns can significantly help people to protect themselves.
It is essential to know how to choose the best isolation gown level for protection. It can be confusing to choose the right quality isolation gown from a multitude of manufacturers.
What Are Isolation Gowns?
An isolation gown protects front-line caregivers from fluid penetration and infectious droplets. It also helps to prevent microorganisms from being transmitted to those with weak immune systems.
Surgical Gowns vs Isolation Gowns:
- Surgical Gown: Any level of risk (Levels 1 through 4) can be covered with surgical gowns. A surgical gown is a personal protective garment that can be worn by healthcare personnel during surgery to protect the patient and the personnel from any possible transmission of microorganisms, fluids, or particulate matter. All surgical gowns must be labeled as “surgical gowns”.
- Surgical Isolation Gowns: Surgical isolation gowns are used when there is a medium to high risk of contamination. For surgical isolation gowns, there is a need for larger critical zones than traditional surgical gowns. All areas of the surgical isolation gown except (bindings, cuffs, and hems) are considered critical zones of protection and must need the highest liquid barrier protection level for the gown. All seams must be protected as well.
- Non-Surgical Gown: Non-surgical gowns are used to protect the wearer from the transfer of microorganisms and body fluids in low or minimal risk patient isolation situations. When there is a medium to high risk of contamination, non-surgical gowns are not worn during surgical procedures, invasive procedures. Non-surgical gowns are like Surgical isolation gowns.
What is the Critical Zone for Surgical Gown?
The barrier requirements for the design and construction of surgical gowns, other protective apparel are based on the anticipated location and degree of liquid contact, given the expected conditions of use. The critical zones include those areas where direct contact with blood, body fluids, and other potentially infectious materials, although areas outside of the critical zones can inadvertently be sprayed or splashed as well.
Critical Protection Zones for Surgical Gowns
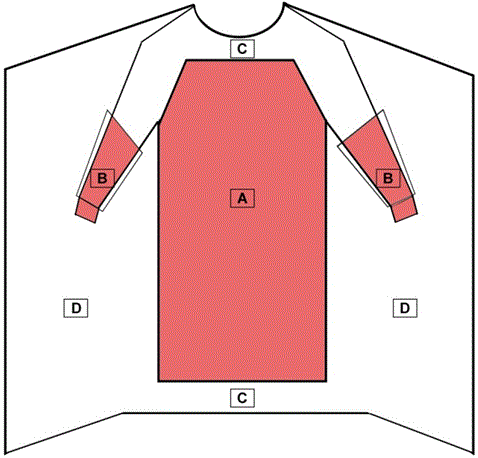
- The entire front of the gown (areas A, B, and C), including the seam and other components, is required to have a barrier performance of at least level 1.
- The critical zone compromises at least areas A and B.
- The back of the surgical gown (area D) may be non-protective.
Example of a surgical gown
- Critical zone — front
- Critical zone — sleeve
- Front
- Back
Source: Critical Zones for Surgical Gowns. (2021, January 13). [Photograph].
Critical Zones for Surgical Isolation Gowns and Non-Surgical Gowns
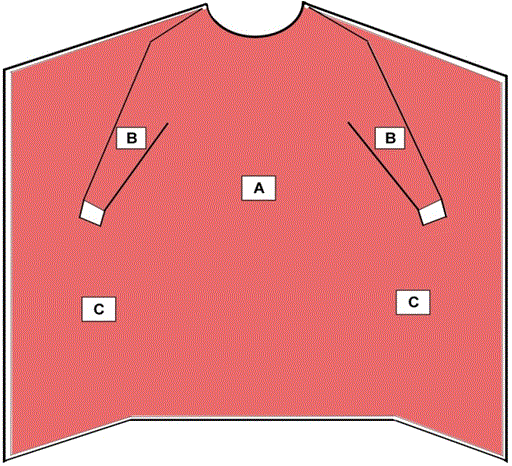
- The entire gown (areas A, B, and C), including seams but excluding cuff, hems, and bindings, is required to meet at least the minimum level 1 of barrier performance.
- When there is a high risk of infection and a need for more critical zones, surgical isolation gowns can be used.
Example of a surgical Isolation gown and non-surgical gown
- Critical zone — front
- Critical zone — sleeve
- Critical zone — back
“Surgical Gowns and Surgical Isolation Gowns are regulated by the FDA as a Class II medical device that requires a 510(k) premarket notification.”
“Non-Surgical Gowns are Class I medical devices (exempt from premarket review)”
The Level of Protection Standards
The standard ANSI/AAMI PB70:2012 created a classification system (Levels 1 through 4) for all apparel used within a healthcare environment. This covers surgical gowns, isolation gowns, and many other items. These standards are required by the FDA for all medical textile manufacturers.
Protective apparel must conform to a set of standards and undergo a specific set of tests to determine “the liquid barrier performance and classification of protective apparel and drapes intended for use in health care facilities.”
Follow the link below to know more about the standards of the US and EU.
What is the standard of medical gowns? 2 differences between USA and EU standards
3 Things to Evaluate When Choosing an Isolation Gown
The Centers for Disease Control (CDC) suggests that you consider three things when choosing gowns for healthcare settings.
Purpose
- Who will be wearing the gown?
- In what setting will they be working?
- What are the possible types of risks?
Answers to those questions determine what type of isolation gowns you need.
Materials – What are isolation gowns made of?
- Disposable isolation gowns are made from polyethylene or polypropylene.
- Reusable isolation gowns are made from cotton or synthetic materials, such as polyester or poly-cotton blend. They can also be latex-free.
Synthetic materials generally do a better job of blocking fluids and are preferred over cotton when it comes to COVID-19 prevention.
Risk Level
The risk level of the environment and type of exposure anticipated determines what types of isolation gowns you should wear.
For example, in a low-risk environment (like a blood draw), the medical professional needs an AAMI, Level 2 gown.
How to Put on and Remove an Isolation Gown?
The ease or difficulty with which a gown is put on and removed may affect its effectiveness and the potential for contamination, especially during the doffing of a contaminated gown.
Put on
- Select appropriate type and size
- The opening is in the back
- Secure at neck and waist
- If a gown is too small, use two gowns for better protection
- Put on the first gown with the opening in front and the second gown over the first with the opening in the back.
Take off
- Unfasten ties
- Peel gown away from neck and shoulder
- Turn contaminated outside toward the inside
- Fold or roll into a bundle (Only the “clean” part of the gown should be visible)
- Discard
Hand hygiene is an important part of the job for Health Care Providers. Hand hygiene can be achieved by using an alcohol-based hand sanitizer containing 60-95% alcohol, or by washing your hands with soap and warm water for at most 20 seconds. Hands that are visibly stained should be washed with soap and water before returning to the alcohol-based hand sanitizer.
How to Choose the Right Isolation Gown to Prevent COVID-19
According to the CDC’s COVID-19 resources, selecting the correct level of isolation gown depends on the protection needed for the circumstances.
Patients
For patients with suspected or confirmed cases of COVID-19, please use non-sterile disposable patient isolation gowns, which are used for routine patient care in healthcare settings.
Medical Professionals
For medical professionals engaging in activities where the risk of bodily fluid exposure is low or minimal, gowns that claim minimal or low-risk levels of barrier protection (ANSI/AAMI PB70 Level 1 or Level 2) can be used.
For situations where medium to high-risk levels of contamination and need for a large critical zone, isolation gowns that claim moderate to high barrier protection (ANSI/AAMI PB70 Level 3 or Level 4) can be used.
Conclusion
Companies might advertise different product names when they are selling isolation gowns (e.g., patient gown, nursing gown, procedural gown, non-surgical gown, etc.) It is important to consider the function and intended use of the product, as well as what level of protection it offers. You will be able to choose the right isolation gown by looking at the description and packaging.
The Product label is more important than the product name.